
Unique Anatomies
Patient-Matched
Solutions
MySpine is a patient-matched pedicle screw placement guide, allowing the surgeon to determine his preoperative 3d planning, based on CT images of the patient’s spine. This innovative concept combines several different features to offer potential benefits to both the surgeon and the patient.
The MySpine guides increase accuracy in screw positioning potentially reducing the risk of pedicles violation.
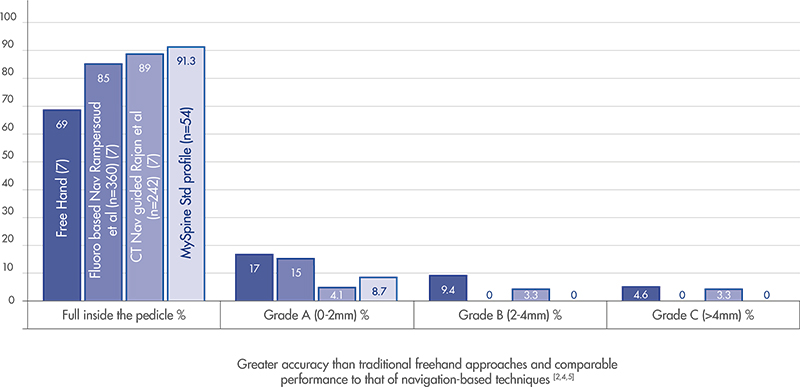
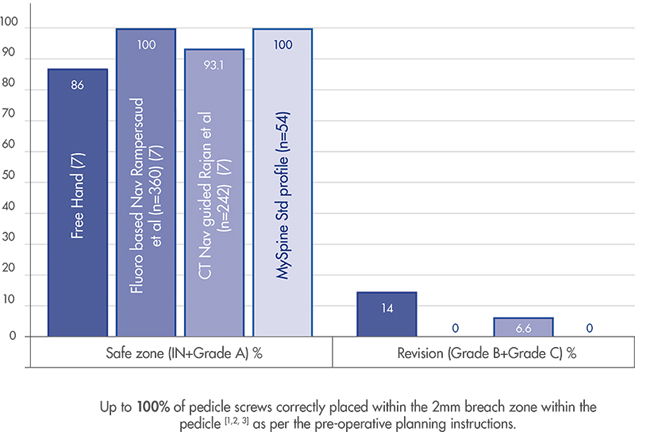
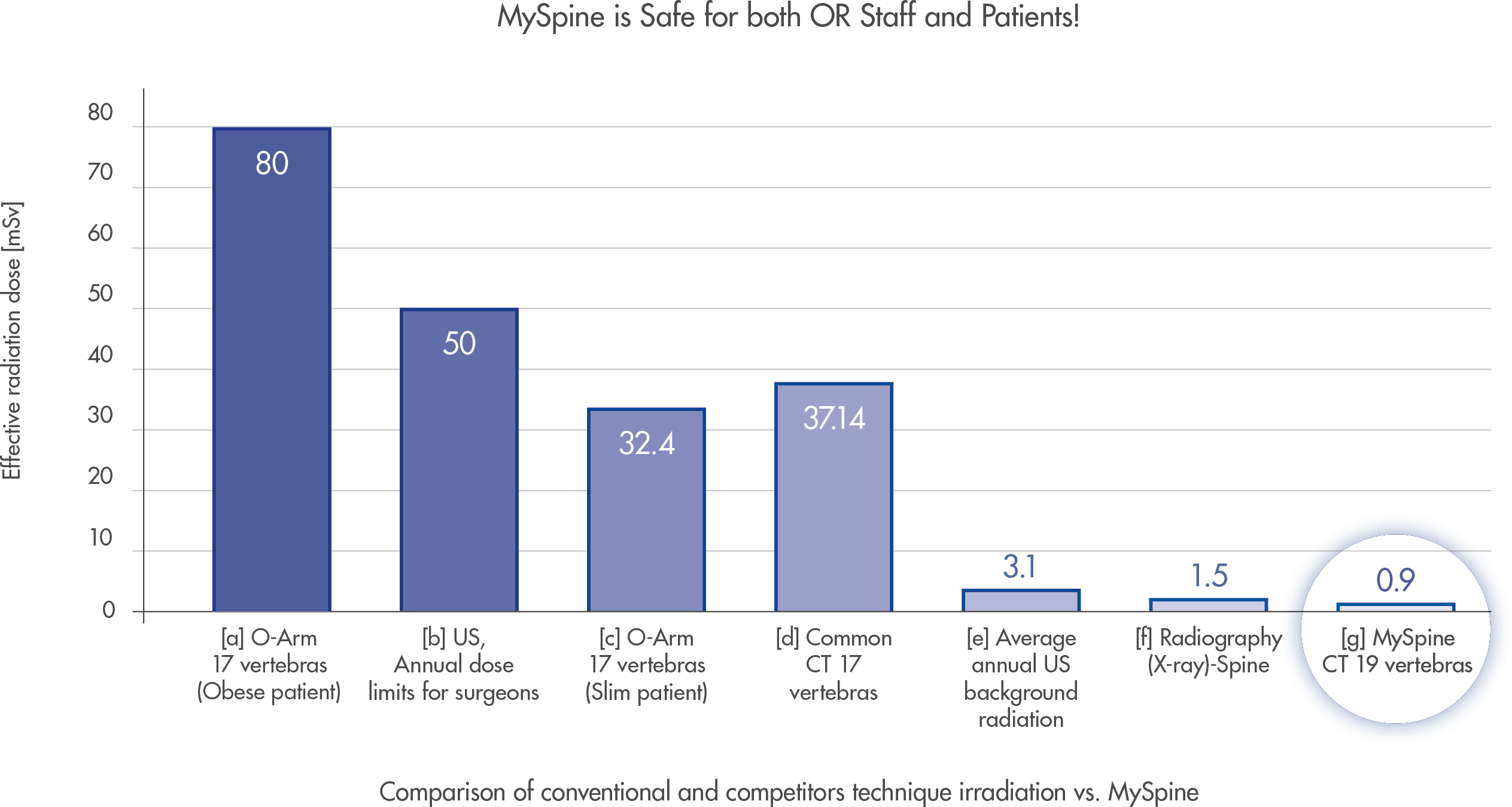
A dedicated MySpine Low Dose CT protocol developed in order to minimize the X-ray exposure for patients, moreover MySpine potentially allow a complete reduction of intraoperative fluoroscopy without sacrificing accuracy[6].
Low dose radiation protocol greatly benefits the patients in comparison to using C-Arm or O-Arm navigational technologies: more than 30 times less irradiation! (c).
Overall dose amount per surgery is up to 50 full spine X-rays less than free-hand technique (data on internal files).
Great results in terms of time and cost reduction can be achieved with the MySpine technology:
Online interactive 3d planning tool for reliable pedicle targeting and screw trajectory identification.
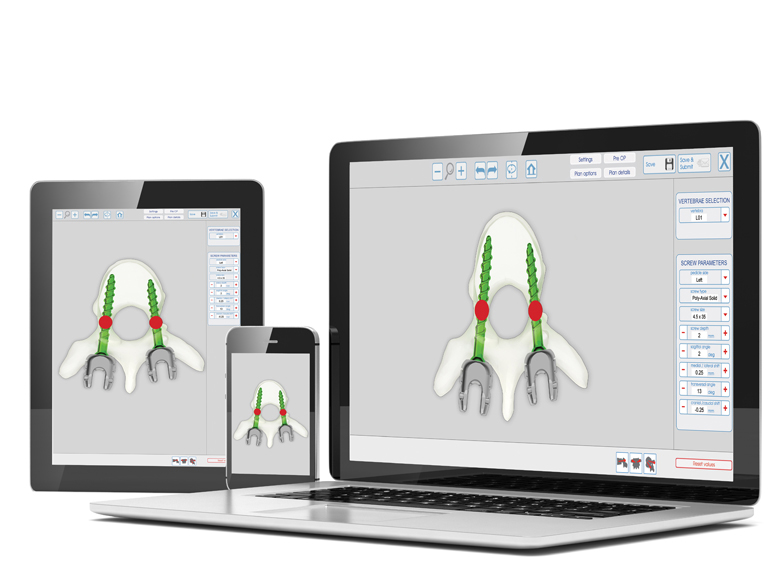

The surgeon determines the entry points for the pedicle screws and sets their trajectory along with the main geometrical parameters.
.jpg)
MySpine guides are positioned on the vertebra using different contact points on distinct anatomical references, such as the spinous and transverse processes, in order to achieve the maximum stability.

MySpine guides are designed to preserve the patient’s anatomy.

Distal windows enhance the field of view during all surgical steps.

Standard MySpine guides are suitable for challenging deformities and long constructs.
.jpg)
Low Profile MySpine guides are ideal for low lumbar regions and degenerative cases where a small incision is preferred.
MySpine MC is a 3D printed patient-matched solution in the midline cortical approach. Posterior lumbar fusion is driven in a minimally invasive [1], muscle sparing way, allowing for shorter operating times [2,3] and a substantial reduction of both radiation exposure [2] and costs [2,3].
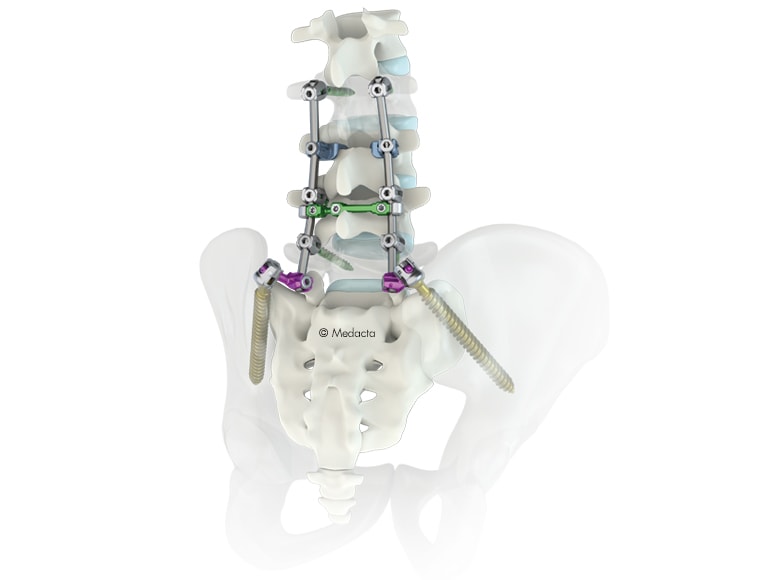
MySpine S2AI screw fixation technique was developed recently to provide increased fixation with a lower profile screw and rod construct[9]. This technique may provide advantages such as decreased rates of reoperation, surgical site infection, wound dehiscence and symptomatic screw prominence as compared to traditional iliac screw fixation.[10]
MySpine pedicle screw placement guides are exclusively intended for use with the Medacta M.U.S.T. pedicle screw system and related instruments when the clinical evaluation complies with the need of spinal fixation.

MyKnee is a patient-matched cutting block, allowing the surgeon to realize his preoperative 3D planning, based on CT or MRI images of the patient’s knee.
This innovative concept combines different features giving potential benefits to both the surgeon and to the patient.

MyShoulder is a patient-matched instrumentation, allowing the surgeon to realize his preoperative 3D planning, based on CT images of the patient’s shoulder. The pre-operative 3D planning allows to manufacture an humeral resection guide and a glenoid positioning guide.This innovative concept combines different features giving potential benefits to both the surgeon and to the patient.
An advanced network of digital solutions designed to improve patient outcomes and healthcare efficiency
MYSPINE PUBLICATIONS
[1] Lamartina et al. Adolescent idiopathic scoliosis surgery with patient-specific screw placement-guide Eur Spine J. 2014 Dec; 23(12)
[2] Lamartina et al. Pedicle screw placement accuracy in thoracic and lumbar spinal surgery with a patient-matched targeting guide: a cadaveric study. Eur Spine J. 2015 Nov;24(7)
[3] Putzier et al. A New Navigational Tool for Pedicle Screw Placement in Patients with Severe scoliosis: A Pilot Study to Prove Feasibility, Accuracy, and Identify Operative Challenges. J Spinal Disord Tech. 2014
[4] Landi et al. Spinal Neuronavigation and 3D-Printed Tubular Guide for Pedicle Screw Placement: A Really New Tool to Improve Safety and Accuracy of the Surgical Technique? J Spine 2015, 4:5
[5] Landi et al. 3D Printed Tubular Guides for Pedicle Screw Placement: The Answer for the Need of a Greater Accuracy in Spinal Stabilization. Orthop Muscular Syst 2015, 4:3
[6] Farshad et. al. Accuracy of patient-specific template-guided vs. free-hand fluoroscopically controlled pedicle screw placement in the thoracic and lumbar spine: a randomized cadaveric study. Eur Spine J. 2016
[9] Sponseller P. et al., “Low Profile Pelvic Fixation With the Sacral Alar Iliac Technique in the Pediatric Population Improves Results at Two-Year Minimum Follow-up”, Spine, September 15, 2010
[10] Ai-Min Wu, et al. “The technique of S2-alar-iliac screw fixation: a literature review“.
8th M.O.R.E. International Symposium Proceedings
A pilot study to prove feasibility, accuracy, and identify operative challenges (Michael Putzier)
MySpine surgical technique - description of technique, challenges & risks (Giovanni Grasso)
My overall impressions as a newest user of MySpine guides (Olivier Ricart)
Radiation safety in orthopaedics and neurosurgery: does the radiation dose matter? (Angus Gray)
SUPPORTING LITERATURE
[7] Gelalis et.al. Accuracy of pedicle screw placement: a systematic review of prospective in vivo studies comparing free hand, fluoroscopy guidance and navigation technique. Euro Spine Journal, 2012
[a]Lange et.al. Estimating the effective radiation dose imparted to patients by intraoperative cone-beam computed tomography in toracolumbar spinal surgery, Spine 2013
[b]US Nuclear Regulatory Commission’s (USNRC)
[c]Lange et.al. Estimating the effective radiation dose imparted to patients by intraoperative cone-beam computed tomography in toracolumbar spinal surgery, Spine 2013
[d]Biswas et.al. Radiation Exposure from Musculoskeletal Computerized Tomographic Scans, JBJS Am. 2009
[e]Health Physics Society Specialists in Radiation Safety, Lawrence Berkeley National Laboratory; Fact Sheet 2010
[f]Radiation Dose in X-Ray and CT Exams; 2013 Radiological Society of North America, Inc
[g]MySpine, Charité University Hospital, Berlin, Germany