
Dislocation remains one of the most common causes of hip revision. Sariali[1] reports dislocation rates of between 0.5% and 10% for primary THA, increasing to between 10% - 25% following revision surgery. Following primary total hip arthroplasty, the treatment of dislocation is often expensive and, in the case of revision surgery, this cost can be as high as 148% of the hospital costs in comparison to an uncomplicated total hip replacement[2].
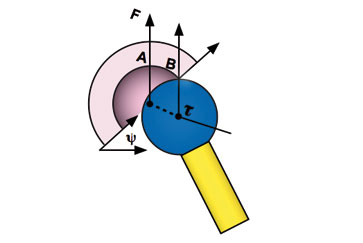
A predictive factor to evaluate effectiveness in dislocation prevention is the jumping distance, which can be defined as the lateral translation (AB) of the centre of the femoral head (τ) before dislocation occurs. F is the load force and ψ is the planar cup inclination angle measured in the frontal plane[3]. The lower the jumping distance, the higher the theoretical risk ofdislocation.
The jumping distance of the Versafitcup® Double Mobility (Medacta®) has been compared with other prosthesis designs aimed as solution for hip instability (cups with a design corresponding to a truncated hemisphere of 165°, such as M2a-MagnumTM (BIOMET)[4] and DUROM (Zimmer); dual mobility cups with a flat design or presenting an opening). Results are shown in the table below: the Versafitcup® Double Mobility has a cup design that provides effective hip stability and has produced better theoretical results than other designs on the market[5].
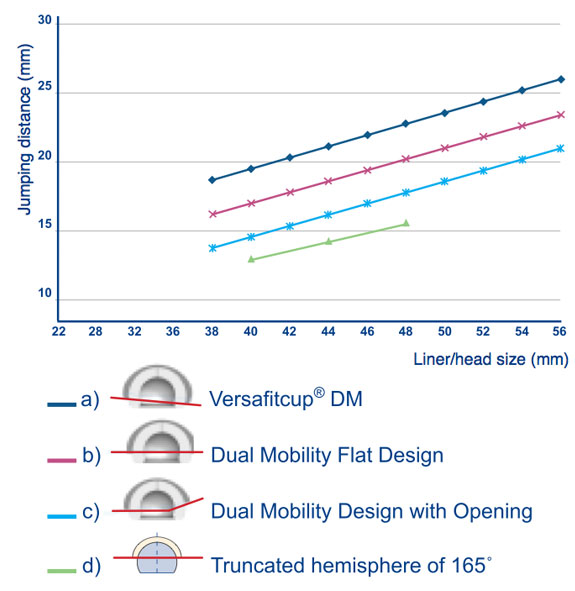
As an example, for heads (or liners in case of dual mobility design) size 48 we calculated the following jumping distance (JD) depending on the design: for Versafitcup® DM the JD is 22.7 mm, for a dual mobility cup with a flat design JD is 20.2 mm, for a dual mobility cup with opening JD is 17.8 mm and for a M-o-M cup (truncated hemisphere of 165°) the JD is 15.8 mm.
The Versafitcup® Double Mobility is the design with the largest jumping distance[5]. These results are reached due to the technical features of the Versafitcup® DM cup:
5° raise, which increases the cover surface of the cup on the liner in the posterior part and enhances the inset value as a result;
The numerical results are supported and validated by clinical studies demonstrating that, after 5 years (minimum) follow-up of over 120 patients, there were no dislocations, no cup migrations, no loosening and no detectable wear[6].

[1] Sariali E, Leonard P, Mamoudy P, “Dislocation after total hip arthroplasty using Hueter anterior approach.” J Arthroplasty 2008; 23 (2): 266-72.
[2] Sanchez-Sotelo J, Haidukewych gJ, Boberg CJ. “Hospital Cost of Dislocation After primary Total Hip Arthroplasty.” J Bone Joint Surg, 2006 Feb, 88(2):290-4.
[3] Sariali E, Lazennec Jy, Khiami F, Catonné y, “Mathematical evaluation of jumping distance in total hip arthroplasty.” Acta orthopaedica 2009; 80 (3): 277-282.
[4] “Design Affects Performance of Metal-on-Metal Constructs.” BioMET orthopedics, Form No. Boi0325.0 RE V063011.
[5] Data on file Medacta®.
[6] Laffargue P, Versafitcup® “Double Mobility cup: outcomes at a mean follow-up of 5 years.” EFFoRT 2011, June 1st to 4th, Copenhagen (DK).
©Medacta International 2017-2025. All Rights Reserved.
All trademarks are property of their respective owners and are registered at least in Switzerland